Pharmacogenetics is a relatively new medical technology that helps ensure that employees suffering from chronic conditions are able to manage those conditions effectively. This increased effectiveness results in lower costs for prescription medications and reduces the duration and, potentially, the frequency of long term disability claims.
What is Pharmacogenetics?
Although an intimidating word, pharmacogenetics is a simple solution to a complex problem. Pharmacogenetic testing determines how a person will respond to certain prescription medications based on their genetic makeup. The test helps people with chronic conditions get on the right medication, at the right dosage, sooner.
Pharmacogenetics is not to be confused with genetic tests used to determine ancestry nor does it predict the likelihood that someone may be susceptible to a particular disease.
Want to learn more about pharmacogenetics?
Watch our video below:
Pharmacogenetic testing focuses on medications used in the treatment of chronic conditions such as heart disease, epilepsy, diabetes, cancer, and mental health conditions such as anxiety and depression. A blood test or a saliva swab is taken to determine if the individual has certain gene variants which affect their reaction to certain medications.

Disclaimer: Not all conditions nor all medications are available for testing.
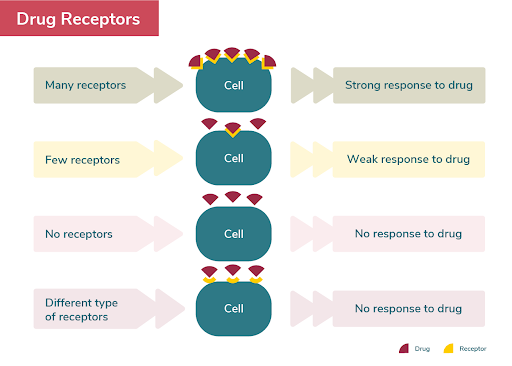
When taking medications, people fall into one of five metabolic groups: ultrarapid, rapid, normal, intermediate, or poor. The same genetic variant can still cause different reactions to different medications for the same condition. In other words, someone may be a poor metaboliser of Drug A but be a rapid metabolizer of Drug B, both of which are used to treat the same type of cancer.
Learning how a person reacts to specific medications for chronic conditions minimises trial and error. When a patient is diagnosed with depression, for example, a physician will prescribe a standard dose of the most commonly used medication. What frequently happens is that the patient starts medicating but suffers from unpleasant side effects or experiences no improvement at all.
The unpleasant side effects may be caused by the patient being a poor metabolizer of the drug, building up a toxic level quite quickly. The lack of improvement could be caused by the patient being a rapid metabolizer, and their body processing the medication so quickly that a standard eight-hour dose leaves their system in two hours.
In both cases, the patient feels frustrated and likely stops taking the medication. This results in repeated visits to the physician until the right drug and/or dosage is found—a process that can take months and may never uncover the right medication.
How Pharmacogenetics Help Control Benefits Costs
There are two primary ways in which pharmacogenetics help control costs. The first is designed to shorten the duration of long-term disability claims in the employee population. The second allows physicians to prescribe medications more precisely, which results in fewer adverse drug reactions and better health for both employees and their dependents.

To date, pharmacogenetic testing has been utilised primarily by insurance companies for plan members on long-term, and sometimes short-term, disability claims. Insurers offer claimants suffering from one of the measurable conditions the opportunity to undergo testing in order to better tailor their treatment plan. A study by Greenshield Canada focused on the use of testing to help treat plan members suffering from mental health conditions. As summarized in a Benefits Canada article, the study found that patients receiving pharmacogenetics-guided treatment reported significantly greater improvements over a six-month period across a range of outcome measurements, including severity of depression and anxiety, as well as level of disability.
Given that mental health conditions such as depression are either the primary reason or a co-morbidity factor in most long-term disability claims, having a tool available which improves outcomes should translate into less pressure on the disability income pools thus resulting in more favourable LTD premiums over time.
The second way pharmacogenetic testing can help control costs is more proactive. Employees or their dependents who are currently suffering from, or recently diagnosed with, a chronic condition can be offered testing. While such tests increase costs in the short term, savings occur due to the overall spend on prescription medications being reduced through the disruption of the trial and error cycle and better drug adherence.
Savings will also occur outside of the benefit plan through a reduction in presenteeism and absenteeism due to improved health.
How Can An Employer Incorporate Pharmacogenetic Testing into Their Benefits Plan?
Pharmacogenetic testing is likely already available to any employee currently receiving short or long-term disability benefits through a Canadian insurer. To expand testing so that it becomes more of a preventative measure, employers can allow the expense to be reimbursed through an Healthcare Spending Account or in some cases, paid through the core plan.
Currently, Life Labs offers genetic testing to individuals for $500. It is expected that as additional players enter the market, the price will fall.
Final Thoughts
According to a study by Express Scripts Canada, the top 5% of claimants are responsible for 52% of prescription drug spend. Most of that spend consists of a long trial and error period to treat a common chronic condition that’s covered by pharmacogenetic testing. Given that your total spend could be reduced, doesn’t it make sense to add this benefit to your employee health plan?

.jpg?height=100&name=Preet%20(1).jpg)






